Levitra enthält Vardenafil, das eine kürzere Wirkdauer als Tadalafil hat, dafür aber schnell einsetzt. Männer, die diskret bestellen möchten, suchen häufig nach levitra kaufen ohne rezept. Dabei spielt die rechtliche Lage in der Schweiz eine wichtige Rolle.
Untitled
For reprint orders, please contact [email protected]
Craniomandibular muscles,
intraoral orthoses and migraine
Elliot Shevel
Intraoral splints are effective in migraine prevention. In this review, changes in the quality of
life of migraineurs treated with a palatal nonoccluding splint were measured. Using the
Migraine Specific Quality of Life Instrument (Version 2.1), it was found that the palatal
nonoccluding splint significantly improved the quality of life of migraineurs. The role of the
craniomandibular muscles in the pathophysiology of migraine is also discussed.
Expert Rev. Neurotherapeutics 5(3), 371–377 (2005)
Migraine is a common disorder with a life-
Materials & method
Materials & method
time prevalence of 16% worldwide, and a
last-year prevalence of 10% [1,2]. It may sig-
In total, 152 patients, 117 female and 35 male,
Discussion
nificantly diminish quality of life, even
were admitted to the study. The inclusion
between attacks, and impairs quality of life
Expert opinion
more than diabetes, hypertension and osteo-
• Age of onset of migraine before 50 years
Five-year view
arthritis [3–5]. Although the pathogenesis of
• Subjects with all or most of their own teeth,
Key issues
migraine headache remains poorly under-
and who did not wear a removable dental
References
stood, current theories suggest a primary,
possibly genetically determined, CNS dys-
Affiliation
function to be involved. There is activation
• History of migraine of 1 year or more, with
of the trigeminovascular system
at least one attack per week in the previous
is comprised of the meningeal vessels,
trigeminal nerve and trigeminal nucleus, in
• Headache free between attacks
particular the trigeminal subnucleus
• A diagnosis of migraine without aura
caudalis [8].
(i.e., group 1.1 in the guidelines laid down
Tenderness and dysfunction of the crani-
by the Headache Classification Committee
omandibular muscles is a common finding
of the International Headache Society)
in migraine [9–15]. Intraoral interocclusal
To make the diagnosis of migraine without
orthoses, used in the treatment of cranio-
aura, the following criteria must be met [27]:
mandibular muscle dysfunction [16–21], arealso effective in preventing migraine
A. At least five attacks fulfilling criteria B, C
Their therapeutic muscle-relaxing effect is
attributed to the fact that they encourage
B. Headache attacks lasting 4–72 h (untreated
the mandible to assume the physiologic rest
or unsuccessfully treated)
position, thereby altering habitual neu-
C. Headache has at least two of the following
The Headache Clinic,
romuscular patterns within the mastica-
characteristics: unilateral location, pulsat-
Suite 256, P Bag X2600,
tory muscles [21]. When a nonoccluding
Houghton, 2014, South Africa
ing quality, moderate or severe intensity
palatal orthosis is worn, there is increased
Tel.: +27 114 840 933
(inhibits or prohibits daily activities),
Fax: +27 114 840 982
resting length and relaxation of the cranio-
aggravated by walking up stairs or similar
mandibular muscles [25,26]. This study
routine physical activity
determined the effect of wearing a nonoc-
KEYWORDS:
D. During the headache at least one of the fol-
craniomandibular, migraine,
cluding palatal orthosis on the quality of
lowing: nausea and/or vomiting,
muscle dysfunction, orthosis
life of migraineurs.
photophobia and phonophobia
2005 Future Drugs Ltd
Factors that could influence the frequency or intensity of
• Role function restriction, which measures the percentage of
migraine, such as pregnancy, the use of prophylactic migraine
time that the patient can perform normal daily activities
medication or ergot derivatives, a history of drug or alcohol
• Role function prevention, which measures the percentage
abuse, or serious illness were exclusion criteria. All participants
productivity while working
were fully informed of the nature of the project and their prior
• Emotional function, which measures the percentage of
consent was obtained.
emotional and relationship disability
Patients completed the MSQ before the start of treatment
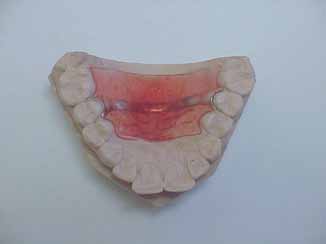
The posture-modifying appliance (PMA) was fabricated using
and again 12 months later. Participants were instructed to
the maxillary cast of the subject. It consisted of a 3 mm thick
continue using palliative medication whenever necessary.
acrylic resin reinforced with a chrome cobalt strip (FIGURE 1).
The appliance covered the hard palate, with the exception of
the anterior part where the tip of the tongue normally touches
As there was no significant statistical difference between the
during speech.
results for males and females, they were combined, and the
The PMA was adjusted for fit and overall comfort. Patients
average pretreatment and post-treatment scores for each
were told that the PMA should not interfere with the free
parameter were calculated. Analysis of the data using the Stu-
movement of the tongue during speech. They were asked to
dent's t-test showed statistically significant improvement in all
speak with the PMA in situ using the words listed in
three parameters. Role function restriction improved from
which are phonetically balanced and designed to test the whole
54.6 to 91% (p < 0.0001), role function prevention improved
range of English sounds in various combinations
from 45.4 to 84.8% (p < 0.0001) and emotional function
was then removed and the part that the tongue had touched
improved from 45.4 to 91.2% (p < 0.0001).
during speech indicated by the patient. The offending acrylicwas ground away and the process repeated, until the patient
was no longer aware of any interference with tongue move-
Migraine is considered to be a neurovascular syndrome, with
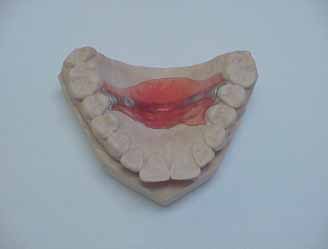
ment. The final shape and thickness of the PMA was, in most
abnormal neuronal excitability in the cerebral cortex, peripheral
patients, very different to the original
sensitization of the trigeminovascular system and pain due to
(FIGURE 2). Subjects were
instructed to wear the PMA day and night, but to remove it
dilation of intracranial blood vessels [30–32]. The triptans were
during tooth brushing, eating and drinking, and when playing
developed as cranial vasoconstrictors to mimic the desirable
contact sports. Subjects were requested to return for adjustment
effects of serotonin [33,34], while avoiding its side effects [35]. An
of the PMA if they experienced discomfort or speech difficulty.
important hindrance to the more widespread use of the triptansis the unsubstantiated perception that they have harmful
Migraine specific quality of life measurement
vasoconstrictor effects [32].
The Migraine Specific Quality of Life Questionnaire (MSQ)
Nociceptive input to the CNS is increased due to sensitiza-
Version 2.1 was used to assess the efficacy of the PMA. The
tion of peripheral sensory afferents, and the resultant barrage of
MSQ is a 14-item, self-administered questionnaire, which
nociceptive impulses results in sensitization of second- and
measures three dimensions of headache-related quality of life
third-order neurons in the CNS. In this way, sensitization may
that are affected by migraine
play a role in the initiation and maintenance of migraine
Consequently, current research has focussed upon prejunctionaland presynaptic targets on nociceptive trigeminovascular neu-rons in an attempt to develop drugs that inhibit trigeminalnociceptive traffic and central sensitization withoutvasoconstrictor effects [32,37].
Central sensitization is induced by nociceptive afferent input
from the intracranial dura mater travelling along thetrigeminovascular pain pathway [38]. It results in [39–41]:
• A reduction of the threshold to cell depolarization
• Cellular activity that continues after cessation of the
peripheral nociceptive input
• A spread of cellular activity to neighbouring cells
Noxious stimulation of muscle afferents also increases the
excitability of spinal cord neurons [42]. Persistent stimulationleads to cellular and molecular changes, which result in neuro-
Figure 1. The posture-modifying appliance before adjusting
nal hyperexcitability, to the extent that pain is elicited by low-
for speech.
threshold, normally non-noxious, stimuli [43–49]. After anincrease in central excitability produced by the activation of
Expert Rev. Neurotherapeutics 5(3), (2005)
Muscles and migraine
peripheral chemoreceptors, cells in the trigeminal nucleus cau-dalis that are normally nociceptive-specific begin to respond to
Box 1. Phonetically balanced word list designed to test
low-threshold, primary afferent non-nociceptive mechano-
the whole range of English sounds in various
receptors [50]. Repeated stimulation of a dorsal root produces,
in some neurons, a prolonged heterosynaptic facilitation withan augmentation of the response to the conditioning root
(homosynaptic potentiation) as well as to adjacent test roots
(heterosynaptic potentiation)
Restoring a patient's ability to function normally is now
recognized as the primary treatment goal, rather than merely
[52]. The results of this study show that relaxa-
tion of the craniomandibular muscles by means of a PMA
improves the quality of life of migraineurs. By reducing sen-
sory input from the craniomandibular muscles, central sen-
sitization is reduced. The probable mechanism is that
intraoral splints may have therapeutic effects apart from
• Volumetric analysis of the masseter and medial pterygoid
those commonly attributed to the occlusal component [53].
muscles showed that the volume of masticatory muscles in
This may be attributed to the fact that an intraoral appli-
migraineurs is nearly 70% greater than in nonmigraineurs
ance may encourage the mandible to assume the physiologic
rest position, thereby altering habitual neuromuscular pat-
terns within the masticatory muscles [54]. Further research
has shown that when a nonoccluding palatal appliance isworn there is an increase in the interocclusal distance and,
• Sensory afferents from the craniomandibular muscles
consequently, in the resting length of the masticatory
project to the trigeminal sensory nuclei, and in particular
muscles [55,56].
to the subnucleus caudalis. Subnucleus caudalis neurons,
A limitation of this study is the lack of a placebo control
including low-threshold mechanoreceptive, wide-dynamic
group. There is, unfortunately, no remedy for this when
range and nociceptive-specific neurons, are excited by the
testing a physical intervention such as an intraoral appli-
stimulation of craniomandibular muscle sensory
ance, given the sensitivity of the intraoral structures. The
possible placebo effect of the PMA cannot therefore be
• The subnucleus caudalis also acts as a critical interneuronal
measured, and its importance must remain the subject of
relay site in craniofacial nociceptive reflex activity involving
speculation. According to Occam's Razor, in science the sim-
the craniofacial muscles [67–70].
plest theory that fits the facts of a problem is the one thatshould be selected. This is interpreted to mean that the sim-
plest of two competing theories is preferable. If Occam's
The following clinical findings have been determined:
Razor is applied, then the most likely conclusion is that the
• Pericranial muscle pain and tenderness are prominent
PMA does have a beneficial nonplacebo effect. The possibil-
features in migraine [71–73]
ity of natural regression of the migraine in this group of
• There is increased pericranial muscle electromyographic
patients is minimal, given that all the subjects had been suf-
activity in migraine
fering for a long time frame without improvement until the
PMA was fitted.
• Physical therapy can precipitate migraine attacks [76]
Further corroborating evidence that the craniomandibular
muscles play a role in the cascade of events in migraine
pathogenesis is described below.
Treatment modalities that reduce craniomandibular muscletension are effective in the treatment of migraine and include:
• Intraoral splints which reduce migraine intensity and
• The middle meningeal artery, dura of the middle and ante-
rior cranial fossae, and craniomandibular muscles, all receive
• Biofeedback to induce muscle relaxation is widely used in
sensory afferents from the mandibular division of the trigem-
migraine prophylaxis. The positive treatment response to
inal nerve. They all send sensory afferent input to the subnu-
biofeedback/relaxation in migraine headache is not related to
cleus caudalis, possibly enhancing central sensitization. The
presence of changes in blood flow velocity [83].
middle meningeal artery and dura of the middle and anterior
• Intramuscular trigger point injections are effective in the
cranial fossae via its recurrent meningeal branch, and the
treatment of acute migraine pain [84–86].
muscles via their individual branches [57,58].
findings suggest a relationship between migraine headaches onthe one hand and dysfunction of the craniomandibular muscleson the other. In this study, the quality of life of migraineurs wassignificantly enhanced by the use of an intraoral palatal nonoc-cluding appliance. This and other evidence, including anatomi-cal evidence, the projection of sensory afferents from the crani-omandibular muscles to the trigeminal subnucleus caudalis,clinical findings, treatment modalities designed to reduce mus-cle tension which also successfully treat migraine, and drug tri-als, provide a compelling argument that central sensitization inmigraineurs is enhanced by sensory input originating from thecraniomandibular muscles. Therefore, the best current treat-ment regimen must include assessment and treatment of thepericranial muscles.
Figure 2. Example of the posture-modifying appliance after adjusting
It is unlikely that this treatment regimen will gain much favor.
for speech.
The reason being that medicine is divided into different disci-plines, each with its own sphere of interest. While the general
• Resection of the corrugator supercillii muscles in patients
public may believe that these disciplines share information at
who respond positively to botulinum toxin A injection
the highest level, in reality they rarely communicate with each
results in prolonged and effective migraine
other. The excellent results achieved with the use of intraoral
splints in migraineurs have been on record for many years. Inspite of this, intraoral splints are rarely mentioned in the
headache literature – there is not a single article on the subject
Preliminary studies indicate that drugs such as botulinum
in Headache or Cephalalgia in at least the last 3 years. Unfor-
toxin A, baclofen and tizanidine, which reduce skeletal mus-
tunately, despite the excellent clinical results, splint therapy
cle spasm and tone, may be useful in migraine
for migraine is still regarded with scepticism. In the words of
prophylaxis [90].
Max Planck (Nobel Prize Physicist, 1918), "A new scientific
Sumatriptan was developed as a cerebral vasoconstrictor, but
truth does not triumph by convincing its opponents and
it has also been shown to act on skeletal muscle [91–93]. It cannot
making them see the light, but rather because its opponents
be excluded, therefore, that the triptans may be effective in
eventually die, and a new generation grows up that is familiar
migraine due to altered muscle metabolism.
with it". It is improbable, therefore, that, despite the provenefficacy of intraoral splints, their use will be widely adopted
within the next 5 years. In the next 50 years. perhaps?
Current theories suggest that a primary, probably geneticallydetermined, CNS dysfunction is involved in the initiation of
the migraine headache, with activation of the trigeminovascular
The author would like to express sincere thanks to Daniel
system and sensitization of neurons in the CNS [6]. Clinical
Shevel for his invaluable input in the writing of this review.
Key issues
• Migraine is a common disorder.
• It is characterized by moderate-to-severe pain, with associated symptoms such as nausea, vomiting, photophobia and phonophobia.
• Migraine is associated with changes in the trigeminovascular system.
• Tenderness and dysfunction of the craniomandibular muscles is a common finding in migraine.
• Intraoral orthoses are used to relax the craniomandibular muscles and restore them to normal function.
• This review studies the effect on migraineurs of wearing a nonoccluding palatal orthosis.
• Placebo-controlled studies are not feasible when intraoral orthoses are used.
• The effect was therefore measured by comparing pretreatment with post-treatment quality of life.
• Statistical analysis of the results showed a significant improvement in quality of life when the orthosis was worn.
Expert Rev. Neurotherapeutics 5(3), (2005)
Muscles and migraine
Olesen J. Some clinical features of the acute
appliance on muscular symptoms in
Papers of special note have been highlighted as:
migraine attack: an analysis of 750 patients.
craniomandibular disorders: a preliminary
Headache 18, 268–271 (1978).
study. J. Craniomandib. Pract. 19, 42–47
•• of considerable interest
Cohen MJ. Psychophysiological studies of
First suggestion in the literature that a
Rasmussen BK, Jensen R, Schroll M,
headache: is there similarity between
palatal appliance could bring about
Olesen J. Epidemiology of headache in a
migraine and muscle contraction headache?
improvement of myofascial pain
general population – a prevalence study. J.
Headache 18, 189–196 (1978).
Clin. Epidemiol. 44, 1147–1157 (1991).
Bakal DA, Kaganov JA. Muscle contraction
Olesen J. Classification and diagnostic
Schwartz BS, Stewart WF, Lipton RB. Lost
and migraine headache: psychophysiologic
criteria for headache disorders, cranial
workdays and decreased work effectiveness
comparison. Headache 17, 208–215
neuralgias, and facial pain. First edition.
associated with headache in the workplace. J.
Cephalalgia 8(Suppl. 7), 19–33 (1988).
Occup. Environ. Med. 39, 320–327 (1997).
Block SL, Apfel M, Laskin DM. The use of
Berger KW. Speech Audiometry Materials.
Gerbaud L, Navez ML, Couratier P et al.
a resilient rubber bite appliance in the
Herald, OH, USA, 46–50 (1977).
Validation of the combined SF36/MSQOL
treatment of MPD syndrome. J. Dent. Res.
test of evaluation of quality of life in
57, A71 (1978).
Patrick DL, Hurst BC, Hughes J. Further
migraine patients in France. Rev. Neurol.
Campbell J. Extension of the
development and testing of the migraine-
158, 719–727 (2002).
temporomandibular joint space by methods
specific quality of life (MSQOL) measure. Headache 40(7), 550–560 (2000).
Michel P, Dartigues JF, Lindoulsi A, Henry
derived from general orthopaedic
Shows that cumulative evidence for the
P. Loss of productivity and quality of life in
procedures. J. Prosthet. Dent. 7, 386–399
migraine-specific quality of life instrument
migraine sufferers among French workers:
meets established criteria for validity,
results from the GAZEL cohort. Headache
Greene CS, Laskin DM. Splint therapy for
consistency and reproducibility. It
37, 71–78 (1997).
the myofascial pain-dysfunction syndrome:
confirmed that quality of life testing is a
Osterhaus JT, Townsend RJ, Gandek B,
a comparative study. J. Am. Dent. Ass. 84,
valid tool for measuring treatment efficacy
Ware JE. Measuring the functional status
624–628 (1972).
in migraine.
and well-being of patients with migraine
Lamey PJ, Steele JG, Aitchison T.
Silberstein SD. Migraine pathophysiology
headache. Headache 34, 337–343 (1994).
Migraine: the effect of acrylic appliance
and its clinical implications. Cephalalgia
Russell MB. Genetic epidemiology of
design on clinical response. Br. Dent. J.
24(Suppl. 2), 2–7 (2004).
migraine and cluster headache. Cephalalgia
180, 137–140 (1996).
Wolff HG. Headache and Other Head Pain.
17, 683–701 (1997).
Matthews E. Treatment for the teeth-
First Edition. Oxford University Press, NY,
Edvinsson L. Aspects on the
grinding habit. Dent. Record 62, 154–155
pathophysiology of migraine and cluster
Goadsby PJ. Prejunctional and presynaptic
headache. Pharmacol. Toxicol. 89, 65–73
Posselt U. Treatment of bruxism by bite
trigeminovascular targets: what preclinical
guards and bite plates. J. Canad. Dent.
evidence is there. Headache Currents 1, 1–6
Goadsby PJ, Lipton RB, Ferrari MD. Migraine
Assoc. 29, 773–778 (1963).
– current understanding and treatment. N.
Quayle AA, Gray RJM, Metcalfe RJ,
Kimball RW, Friedman AP, Vallejo E. Effect
Engl. Med. J. 346, 257–270 (2002).
Guthrie E, Wastell D. Soft occlusal splint
of serotonin in migraine patients. Neurology
Lipchik GL, Holroyd KA, Talbot F, Greer
therapy in the treatment of migraine and
10, 107–111 (1960).
M. Pericranial muscle tenderness and
other headaches. J. Dent. 18, 123–129
Lance JW, Anthony M, Hinterberger H.
exteroceptive suppression of temporalis
The control of cranial arteries by humoural
muscle activity: a blind study of chronic
Lapeer GL. Reduction of the painful
mechanisms and its relation to the migraine
tension-type headache. Headache 37,
sequelae of migraine headache by use of the
syndrome. Headache 7, 93–102 (1967).
368–376 (1997).
occlusal diagnostic appliance: an
Raises the possibility that pericranial
hypothesis. J. Craniomandib. Pract. 6,
Humphrey PPA, Feniuk W, Perren MJ,
muscle tenderness is present early in
82–86 (1988).
Beresford IJM, Skingle M, Whalley ET.
migraine without aura, and thus may
As early as 1988, Lapeer suggested that
Serotonin and migraine. Ann. NY Acad. Sci.
contribute to the etiology.
"further research into occlusal splint
600, 587–598 (1990).
Steele JG, Lamey PJ, Sharkey SW, Smith
therapy as an adjunct to relieving or
Bendtsen L. Sensitization: its role in
GMR. Occlusal abnormalities, pericranial
aborting the painful sequelae of migraine
primary headache. Curr. Opin. Investig.
muscle and joint tenderness and tooth wear
headaches is necessary".
Drugs 3, 449–453 (2002).
in a group of migraine patients. J. Oral
Lamey PJ, Barclay SC. Clinical
Elucidated the concept that nociceptive
Rehabil. 18, 453–458 (1991).
effectiveness of occlusal splint therapy in
input to the CNS may be increased due to
activation or sensitization of peripheral
Lous I, Olesen J. Evaluation of pericranial
patients with classical migraine. Scot. Dent.
tenderness and oral function in patients
J. 32, 11–12 (1987).
with common migraine, muscle
Young P. A cephalometric study of the
Ramadan NM, Buchanan MS, Stare H,
contraction headaches, and combination
effect of acrylic test palatal piece thickness
Pearlman H. Peripheral and central
headache. Pain 12, 385–393 (1982).
on the physiologic rest position. J.
targets for acute migraine therapy: early clinical trial results. Headache Cur. 1,
Tfelt-Hansen P, Lous I, Olesen J.
Philippine Dent. Ass. 19, 5–15 (1966).
7–12 (2004).
Prevalence and significance of muscle
Minagi S, Shimamura M, Sato T, Natsuaki
tenderness during common migraine
N, Ohta M. Effect of a thick palatal
Malick A, Burstein R. Peripheral and
attacks. Headache 21, 49–54 (1981).
central sensitization during migraine.
Funct. Neurol. 15(Suppl. 3), 28–35
Wenzel R, Dortch M, Cady R, Lofland JH,
Sessle BJ, Hu JW, Amano N, Zhong G.
Diamond S. Migraine headache
Convergence of cutaneous, tooth pulp,
Woolf CJ, Salter MW. Neuronal plasticity:
misconceptions: barriers to effective care.
visceral, neck and muscle afferents onto
increasing the gain in pain. Science 288,
Pharmacotherapy 24, 638–648 (2004).
nociceptive and non-nociceptive neurones
1765–1768 (2000).
Greene CS, Laskin DM. Splint therapy for
in trigeminal subnucleus caudalis (medullary dorsal horn) and its
Coderre TJ, Katz J. Peripheral and central
the myofascial pain-dysfunction syndrome:
implications for referred pain. Pain 27,
hyperexcitability: differential signs and
a comparative study. J. Am. Dent. Ass. 84,
219–235 (1986).
symptoms in persistent pain. Behav. Brain
624–628 (1972).
Sci. 20, 404–419 (1997).
Posselt U. Treatment of bruxism by bite
Amano N, Hu JW, Sessle BJ. Responses of neurons in feline trigeminal subnucleus
Dubner R. Neural basis of persistent pain:
guards and bite plates. J. Canad. Dent.
caudalis (medullary dorsal horn) to
sensory specialization, sensory modulation,
Assoc. 29, 773–778 (1963).
cutaneous, intraoral, and muscle afferent
and neuronal plasticity. In: Progress in Pain
Young P. A cephalometric study of the
stimuli. J. Neurophysiol. 55, 227–243
Research and Management. Jensen TS,
effect of acrylic test palatal piece thickness
Turner JA, Weisenfeld-Hallin Z (Eds).
on the physiologic rest position. J.
IASP Press, WA, USA, 77–91 (1997).
Philippine Dent. Ass. 19, 5–15 (1966).
Matthews B. Peripheral and central aspects of trigeminal nociceptive systems. Philos. Trans. R.
Hu JW, Sessle BJ, Raboisson P, Dallel R,
Minagi S, Shimamura M, Sato T, Natsuaki
Soc. Lond. Biol. Sci. 19, 313–324 (1985).
Woda A. Stimulation of craniofacial muscle
N, Ohta M. Effect of a thick palatal
afferents induces prolonged facilitatory
appliance on muscular symptoms in
Tsai C. The caudal subnucleus caudalis
effects in trigeminal nociceptive brain-stem
craniomandibular disorders: a preliminary
(medullary dorsal horn) acts as an
neurones. Pain 48, 53–60 (1992).
study. J. Craniomandib. Pract. 19, 42–47
interneuronal relay site in craniofacial nociceptive reflex activity. Brain Res. 826,
Jensen TS. Mechanisms of neuropathic
293–297 (1999).
pain. In: Pain 1996, an Updated Review.
Shankland WE. The trigeminal nerve. Part
Campbell JN (Ed.). IASP Press, WA, USA,
IV: the mandibular division. J.
Tsai CM, Chiang CY, Yu XM, Sessle BJ.
77–86 (1996).
Craniomandib. Pract. 19, 153–161 (2001).
Involvement of trigeminal subnucleus caudalis (medullary dorsal horn) in
Jensen TS. Recent advances in pain
Asfat R. A review of the neurovascular
craniofacial nociceptive reflex activity. Pain
research: implications for chronic headache.
supply of the mandible. S. Afr. Dent. J. 57,
81, 115–128 (1999).
Cephalalgia 21, 765–769 (2001).
414–416 (2002).
Cairns BE, Sessle BJ, Hu JW.
Gracely RH, Lynch SA, Bennett GJ.
Lamey PJ, Burnett CA, Fartash L, Clifford
Temporomandibular-evoked jaw muscle
Painful neuropathy: altered central
TJ, McGovern JM. Migraine and
reflex: role of brain stem NMDA and non-
processing, maintained dynamically by
masticatory muscle volume, bite force, and
NMDA receptors. Neuroreport 12,
peripheral input. Pain 51, 175–194 (1992).
craniofacial morphology. Headache 41,
1875–1878 (2001).
Gottrup H, Nielsen J, Arendt-Nielsen L,
49–56 (2001).
Steele JG, Lamey PJ, Sharkey SW, Smith G.
Jensen TS. The relationship between
The volume of masticatory muscles in
Occlusal abnormalities, pericranial muscle
sensory thresholds and mechanical
migraineurs is nearly 70% greater than in
and joint tenderness and tooth wear in a
hyperalgesia in nerve injury. Pain 75,
nonmigraineurs (p < 0.0001).
group of migraine patients. J. Oral Rehabil.
321–329 (1998).
Yamakami Y. Characteristics of responses in
18, 453–458 (1991).
Gottrup H, Andersen J, Arendt-Nielsen L,
the trigeminal subnucleus caudalis and
Jensen K, Tuxen C, Olesen J. Pericranial
Jensen TS. Psychophysical examination of
adjacent reticular formation evoked by the
muscle tenderness and pressure-pain
patients following operation for cancer
stimulation of the masseter muscle. Showa
threshold in the temporal region during
mammae. Pain 87, 275–284 (2000).
Shigakkai Zasshi 9, 130–135 (1989).
common migraine. Pain 35, 65–70 (1988).
Koltzenburg M. Painful neuropathies.
Arvidsson J, Raappana P. An HRP study of
Anttila P, Metsahonkala L, Mikkelsson M et
Curr. Opin. Neurol. 67, 307–316 (1998).
the central projections from primary sensory neurons innervating the rat masseter muscle.
al. Muscle tenderness in pericranial and
Yamamura H, Malick A, Chamberlin NL,
Brain Res. 20, 111–118 (1989).
neck-shoulder region in children with
Burstein R. Cardiovascular and neuronal
headache. A controlled study. Cephalalgia
responses to head stimulation reflect central
Shigenaga Y, Sera M, Nishimori T et al.
22, 340–344 (2002).
sensitization and cutaneous allodynia in a
The central projection of masticatory
Clifford T, Lauritzen M, Bakke M, Olesen
rat model of migraine. J. Neurophysiol. 81,
afferent fibers to the trigeminal sensory
J, Moller E. Electromyography of
479–493 (1999).
nuclear complex and upper cervical spinal cord. J. Comp. Neurol. 22, 489–507 (1988).
pericranial muscles during treatment of
Woolf CJ, Shortland P, Sivilotti LG.
spontaneous common migraine attacks.
Sensitization of high mechanothreshold
Luo P, Wong R, Dessem D. Projection of
Pain 14, 137–147 (1982).
superficial dorsal horn and flexor motor
jaw-muscle spindle afferents to the caudal
Burnett CA, Fartash L, Murray B,
neurones following chemosensitive primary
brainstem in rats demonstrated using
Lamey PJ. Masseter and temporalis
afferent activation. Pain 58, 141–155 (1994).
intracellular biotinamide. J. Comp. Neurol. 17, 63–78 (1995).
muscle EMG levels and bite force in
Woolf CJ, Thompson SW, King AE.
migraineurs. Headache 40, 813–817
Prolonged primary afferent induced
Luo P, Dessem D. Inputs from identified
alterations in dorsal horn neurones, an
jaw-muscle spindle afferents to
Blau JN, MacGregor EA. Migraine and the
intracellular analysis in vivo and in vitro. J.
trigeminothalamic neurons in the rat: a
neck. Headache 34, 88–90 (1994).
Physiol. 83, 255–266 (1988–89).
double-labeling study using retrograde HRP and intracellular biotinamide. J.
Lamey PJ, Barclay SC. Clinical
Comp. Neurol. 27, 50–66 (1995).
effectiveness of occlusal splint therapy in
Expert Rev. Neurotherapeutics 5(3), (2005)
Muscles and migraine
patients with classical migraine. Scott. Med.
Vasudeva S, Claggett AL, Tietjen GE,
Freitag FG. Preventative treatment for
J. 32, 11–12 (1987).
McGrady AV. Biofeedback-assisted
migraine and tension-type headaches: do
Lamey PJ, Steele JG, Aitchison T.
relaxation in migraine headache:
drugs having effects on muscle spasm and
Migraine: the effect of acrylic appliance
relationship to cerebral blood flow velocity
tone have a role? CNS Drugs 17, 373–381
design on clinical response. Br. Dent. J. 24,
in the middle cerebral artery. Headache 43,
137–140 (1996).
245–250 (2003).
Emre S, Erdem SR, Tuncer M. Does
Shankland WE. Nociceptive trigeminal
Tfelt-Hansen P, Lous I, Olesen J.
serotonin relax the rat anococcygeus muscle
inhibition–tension suppression system: a
Prevalence and significance of muscle
via 5-HT7 receptors? Naunyn Schmiedebergs
method of preventing migraine and tension
tenderness during common migraine
Arch. Pharmacol. 362, 96–100 (2000).
headaches. Compend. Contin. Educ. Dent.
attacks. Headache 21, 49–54 (1981).
Boska MD, Welch KM, Schultz L, Nelson
23, 105–108 (2002).
Hay KM. Pain thresholds in migraine.
J. Effects of the anti-migraine drug
Shankland WE II. Migraine and tension-
Practitioner 222, 827–833 (1981).
sumatriptan on muscle energy metabolism:
type headache reduction through
Hay KM. The treatment of pain trigger
relationship to side-effects. Cephalalgia 20,
pericranial muscular suppression: a
areas in migraine. J. Roy. Coll. Gen. Pract.
39–44 (2000).
preliminary report. J. Craniomandib. Pract.
26, 372–376 (1981).
Gobel H, Krapat S, Dworschak M, Heuss
19, 269–278 (2001).
Guyuron B, Varghai A, Michelow BJ, Davis
D, Ensink FB, Soyka D. Exteroceptive
Shankland WE. Nociceptive trigeminal
J. Corrugator supercilii muscle resection
suppression of temporalis muscle activity
inhibition–tension suppression system: a
and migraine headaches. Plast. Reconstr.
during migraine attack and migraine
method of preventing migraine and tension
Surg. 106, 429–434 (2000).
interval before and after treatment with
headaches. Compend. Contin. Educ. Dent.
sumatriptan. Cephalalgia 14, 143–148
Guyuron B, Tucker T, Davis J. Surgical
22, 1075–1080 (2001).
treatment of migraine headaches. Headache
Quayle AA, Gray RJM, Metcalfe RJ,
43, 302–303 (2003).
Guthrie E, Wastell D. Soft occlusal splint
Guyuron B, Kriegler JS, Davis J, Amini SB.
therapy in the treatment of migraine and
Elliot Shevel, BDS, Dip, MFOS, MB, BCh
Comprehensive surgical treatment of
other headaches. J. Dent. 18, 123–129
The Headache Clinic, Suite 256, P Bag X2600,
migraine headaches. Plast. Reconstr. Surg.
Houghton, 2014, South Africa
115(1), 1–9 (2005).
Tel.: +27 114 840 933Fax: +27 114 840 [email protected]
Source: http://www.headclin.co.za/uploads/ftp/DrShevelPublications/EXPERT_REVIEW_OF_NEUROTHERAPEUTICS.pdf
AGGIORNAMENTI IN MEDICINA VETERINARIA :questioni di clinica medica degli animali da compagnia Diagnosi caso 1: Il cane magro con il "pancione": un segno, tante cause Grazie alla raccolta anamnestica, la visita clinica e le indagini collaterali è stato possibile raggiungere la diagnosi di sospetto: epatite cronica di origine tossica causata dall'ingestione di parti velenose di Cycas Revoluta. Le epatiti croniche del cane, sono processi flogistici che si sviluppano principalmente a livello del parenchima epatico, con il conseguente innalzamento dei valori delle transaminasi. Si tratta di patologie che si riscontrano soprattutto in cani di età adulta (4-7 anni) ad eccezione delle forme ereditarie da accumulo di rame che possono insorgere anche in soggetti più giovani; risultano maggiormente interessate le femmine, e, pur potendo interessare tutte le razze, esiste maggiore predisposizione per Bedlington Terrier, Dalmata, Labrador Retriever, Whest Highland White Terrier, Dobermann e Spaniel. Dal punto di vista sintomatologico, i cani affetti da epatite cronica possono presentarsi asintomatici o con segni clinici del tutto aspecifici, quali poliuria e polidipsia, anoressia/disoressia, dimagramento, abbattimento e intolleranza agli sforzi, vomito, diarrea e nei, casi gravi, ascite, coagulopatie ed encefalopatia epatica. La visita clinica del paziente raramente porta al riscontro di qualche reperto indicativo ad eccezione di uno scadimento delle condizioni generali del soggetto, o condizioni più eclatanti come ittero o ascite. Anche le alterazioni di laboratorio risultano non sempre indicative: si riscontrano di norma aumenti delle transaminasi , meno costanti aumenti di fosfatasi alcalina e γ-glutamiltransferasi; nelle fasi avanzate è poi possibile evidenziare tutte le alterazioni indicative di un malfunzionamento epatico, come ipoalbuminemia, riduzione dei valori dell'urea, aumento degli acidi biliari, abbassamento del fibrinogeno. Tra le alterazioni ematologiche che si possono incontrare, ci sono lieve anemia, leucocitosi e piastrinopenia (da consumo, in associazione a coagulopatia) oltre all'aumento dei tempi coagulativi (tempo di protrombina (PT), e tempo di tromboplastina parziale, PTT). La diagnostica per immagini, ed in particolare l'ecografia addominale, può solo completare il quadro ma non fornisce la diagnosi di certezza, in quanto possono sia essere evidenziate alterazioni nella struttura epatica, soprattutto in caso di cirrosi, ma non necessariamente soggetti affetti da epatite cronica presentano alterazioni dell'ecostruttura rilevabili all'esame. Lo strumento diagnostico più indicato in caso di tali patologie, è rappresentato dall'esame istopatologico di un campione prelevato tramite biopsia (ovviamente va ricordato che, in caso di patologia avanzata, in cui fossero comparsi deficit coagulativi, quest'ultima risulta controindicata). Nel presente caso l'esame bioptico ed istopatologico non è stato eseguito in quanto il proprietario non ha dato il suo consenso alla procedura perché preoccupato degli elevati rischi anestesiologici dovuti alla grave condizione clinica del suo cane.
More than twenty years ago, four college students asked each other: What if we could offer children from under-resourced communities individualized attention before they enter kindergarten, giving them the critical academic and social skills—the ‘jumpstart'—they need to succeed? The idea took hold and by 2015, Jumpstart had trained more than 40,000 college students and community volunteers, preparing over 87,000 children for kindergarten success. Jumpstart's program is replicated across the country in 14 states and the District of Columbia. We leverage partnerships with higher education institutions, Head Start, community-based preschools, and school districts to create sustainable solutions in order to close the kindergarten readiness gap.


