Levitra enthält Vardenafil, das eine kürzere Wirkdauer als Tadalafil hat, dafür aber schnell einsetzt. Männer, die diskret bestellen möchten, suchen häufig nach levitra kaufen ohne rezept. Dabei spielt die rechtliche Lage in der Schweiz eine wichtige Rolle.
456-z-umb_nardini.qxd
Eur Arch Otorhinolaryngol (2002) 259 : 279–284DOI 10.1007/s00405-002-0456-z
L.Guarda-Nardini · R. Tito · A. Staffieri · A. Beltrame
Treatment of patients with arthrosis of the temporomandibular joint by infiltration of sodium hyaluronate: a preliminary study
Received: 20 June 2001 / Accepted: 25 January 2002 / Published online: 24 April 2002
Springer-Verlag 2002
Abstract Patients with degenerative disease of the tem-
easy technique proved to be valid and lasting. This infil-
poromandibular joint (TMJ) who did not respond to con-
tration technique using sodium hyaluronate looks very
servative medical therapy (splint therapy, selected grind-
promising for patients affected by symptomatic DJD who
ing or physiotherapy) can be treated by arthrocentesis,
do not respond to conservative medical therapy, reflecting
which is associated with intra-articular injections of so-
similarly encouraging findings in the orthopaedic treat-
dium hyaluronate (Hyalgan). In this study, we treated ten
ment of degenerative knee pathology.
dysfunctional patients with degenerative joint disease(DJD) who had been diagnosed clinically and had had the
Keywords Temporomandibular joint · Degenerative
diagnosis confirmed by MRI. All subjects presented im-
joint disease · Arthrocentesis · Sodium hyaluronate ·
paired mouth opening, joint pain at rest and on movement
and impaired masticatory efficiency. We performed onecycle of five infiltrations with joint arthrocentesis and theinjection of sodium hyaluronate at weekly intervals. The
following parameters were assessed before and after infil-tration and at follow-up after 6 months: mouth opening
Sodium hyaluronate, a glycosaminoglycan produced and
(with a mean of between 36.5 mm and 41.9 mm); side-
released by specialised synovial cells, is present in partic-
ways movements (to the right 4.9 mm to 8.9 mm and to
ularly high concentrations in the joint cartilage and syno-
the left 4.7 mm to 9.2 mm); pain at rest (VAS=1.8 to 0.5)
vial fluid. In normal conditions, this substance plays an
and on movement (VAS=7.8 to 1.1); masticatory effi-
important role in maintaining intra-articular homeostasis:
ciency (VAS=5.7 to 8.6); subjective judgement of the
it favours the elasticity and viscosity of the synovial fluid,
functional TMJ limitation level (from 2.8 to 0.8); judge-
providing a cushion against any shocks; it has a lubricat-
ment of efficacy (from 2.4 to 3.2); judgement of tolerabil-
ing, anti-inflammatory and pain-relieving action and en-
ity to the therapy (from 2.0 to 3.1). The therapeutic bene-
ables the tissue repair processes to be activated in the car-
fits observed can be attributed both to joint arthrocentesis
tilage with a normalising action on the synthesis of endo-
and to the characteristics of sodium hyaluronate itself. All
genous acid by the synovial cells [1].
the parameters considered revealed a statistically signifi-
In the presence of osteoarthrosis, the concentration and
cant positive variation that persisted over time (
P<0.05).
molecular weight of sodium hyaluronate in the synovial
The results obtained by this minimally invasive, fast and
fluid are diminished as a consequence of the dilution,fragmentation and production of acid molecules with alower weight than normal, thus compromising the condi-tions of homeostasis [2]. In order to overcome this prob-
L. Guarda-Nardini (✉) · R. Tito
lem, a treatment has been devised whereby the pathologi-
Department of Medicine and Surgery, University of Padua,
cal fluid is removed from the joint and exogenous sodium
hyaluronate is infiltrated, thus bringing the concentration
e-mail:
[email protected], Tel.: +347-358-3259
and molecular weight of the synovial fluid back to nor-mal. This kind of treatment is called viscosupplementa-
tion [3] and has already been used for many years to treat
Department of Ear, Nose and Throat, University of Padua, Padua, Italy
degenerative knee pathology [4, 5, 6].
Sodium hyaluronate injection has also been proposed
for the treatment of TMJ symptomatic degenerative dis-
Department of Dentistry and Stomatology, University of Padua, Padua, Italy
ease that has failed to respond to conservative medical
and physical therapies. This minimally invasive therapeu-
tesis is complete, 1 cc of Hyalgan is injected into the joint, and the
tic approach using arthrocentesis and infiltration aims to
two needles are removed.
During treatment, the mouth opening is monitored before and
restore the protective function of the synovial fluid, nor-
after each infiltration. Assessments are then made of the presence
malising the concentration and molecular weight of the
or absence of pain when chewing food and at rest and of the pa-
sodium hyaluronate [7].
tient's masticatory efficiency before each infiltration. Even thefunctional limitation level of the joint is assessed after each ad-ministration. The patient's judgement about the efficacy of thetherapy and the tolerability of the infiltration procedure itself are
Materials and methods
also recorded. In the follow-up period, the patients are again assessed on the basis of all the chosen parameters at 1, 3 and
In this study, ten patients suffering from DJD (nine women and
6 months after the last of the five infiltrations. During the whole
one man, age range: 39–68 years, mean age: 49.3 years) underwent
period of the five infiltrations, patients followed a physiotherapy
one cycle of five infiltrations [8, 9] of sodium hyaluronate (Hyal-
program of guided mouth opening that went on for 4 weeks after
gan from Fidia S.p.A.) into one or both of the TMJ, with a total of
the last injection.
15 joints being infiltrated according to the protocol in use for thetreatment of degenerative knee pathology [10, 11, 12, 13].
Before being treated with infiltration, all of the patients in-
volved in this study had undergone splint therapy, physiotherapy
or selected grinding without success. All persons gave their in-formed consent prior to being treated. The treatment with Hyalganwas always preceded by arthrocentesis of the upper joint cavity
After the cycle of infiltrations it was possible to note that
with Ringer-lactate solution.
spontaneous opening of the mouth had improved in each
The patients presented degenerative disease with pain, crepitus
of the patients who had been treated by a minimum of
in the joint and impaired mouth opening and masticatory effi-ciency. The examinations performed were a panoramic radiograph
1 mm to a maximum of 9 mm, with a mean increase of
and a MRI of the TMJ with the mouth both opened and closed on
4.9 mm, passing from an initial mean value of 36.5 mm to
the sagittal and coronal planes.
41.4 mm at the end of treatment. At 1 month, opening re-
Before proceeding with the infiltration, various parameters
mained at a mean value of 42.7 mm, and at 3 months, it
were assessed, such as the maximal mouth opening, the sidewaysmovements of the jaw, the presence of pain at rest and when chew-
was 42.5. At 6months, the mean value reached 41.9 mm,
ing food (assessed by VAS), masticatory efficiency and the func-
slightly lower than the mean values at 1 and 3 months, but
tional limitation level during usual jaw movements [8, 11, 14, 15].
still higher than the initial mean values. The maximal
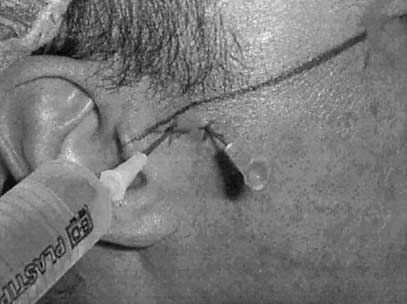
The technique used to perform arthrocentesis of the TMJ (Fig. 1)
mean opening value was achieved 1 month after therapy,
employs the same reference points as are used in arthroscopic ex-amination [16]. The skin surface is disinfected with povidone io-
and at 6 months, the mean value was still higher than the
dine. Local anaesthesia is then achieved with mepivacaine 2%
value obtained at the end of treatment (see Fig. 2). Statis-
(Carbocaine). The anaesthetic is first injected into the joint cavity,
tical analysis (ANOVA) confirmed that over the course of
relaxing this virtual space. Subsequently, the needle is withdrawn
time the cycle of infiltrations favours an improvement in
gently to the skin surface, thus anaesthetising the soft tissues over
mouth opening (P=0.001, P<0.05).
the joint, too. Two 19 G needles are then placed to make entry andexit points for the liquid to be injected that will wash out the entire
Sideways movements of the jaw to the left and right
joint. The arthrocentesis (with 50 cc of Ringer lactate) eliminates
were assessed in terms of time, the side affected by the
the catabolytes present in the synovial fluid [13].
disorder (left, right or bilateral TMJ) and the direction of
This procedure may often prove difficult if the inner part of the
movement. At baseline, the right side gave a mean value
joint shows debris. However, the pressurising effect exercised bythe injection of fluid into the joint is useful in weakening and
of 4.9 mm, while mean movement to the left was 4.7 mm.
breaking up any such debris that may be present. Once arthrocen-
At the end of the therapy, movement to the right had
increased on average by 4.4 mm, reaching a mean valueof 9.3 mm, while the left side had increased by 4.1 mm,reaching a mean value of 8.8 mm. After 1 month, this in-crease had slightly decreased (P=0.000000, P<0.05).
At 3 months, sideways movement had further decreased
to a mean value of 8.6 mm on both sides, increasing againafter 6 months to a mean value of sideways movement tothe right of 8.9 mm and to the left of 9.2 mm. Variationsat follow-up showed a range of less than ±1 mm, demon-strating substantial stability in the results obtained.
Pain at rest was present before treatment in five pa-
tients and was assessed as a mean VAS value of 1.8. Afterthe treatment, the mean value had decreased to VAS=0.8.
After 1 month, the mean value was VAS=0.2. After 3 months, the mean VAS value was 0.1. At 6 months, ithad slightly increased to 0.5. The statistical significancewas equal to P=0.0169 (P<0.05).
Pain on movement was present in all the patients, with
a mean value of VAS=7.8. Symptomatology improved af-
Fig. 1 Technique applied
ter treatment in all cases, with a mean value of VAS=1.6.
Fig. 2 The opening of the
mouth improves after each sin-
gle injection, and there is sub-
stantial preservation of time
during the following 6 months
At 1 month, it had improved to a mean value of VAS=1.2.
patients' masticatory efficiency had reached a mean value
After 3 months, a mean value of VAS=0.8 had been
of VAS=8.7, and at 6 months it had slightly decreased to a
reached. The next control at 6 months showed an absence
mean value of VAS=8.6 (see Fig. 4). ANOVA showed the
of pain in seven patients out of the ten who had received
presence of statistical significance in the data obtained
treatment, with a mean value of VAS=1.1 (see Fig. 3).
with P=0.00000 (P<0.05).
ANOVA showed the presence of statistical significance in
The efficacy judgement of the therapy expressed by
the data obtained (P=0.00000, P<0.05).
the patient was measured numerically (0=poor, 1=slight,
The patients' masticatory efficiency was assessed be-
2=moderate, 3=good and 4=excellent) after each infiltra-
fore treatment and gave a mean value of VAS=5.7, which
tion. After the first infiltration, the mean efficacy value
meant they had considerable difficulty in eating hard,
was 2.4. The mean values increased progressively in the
solid food. At the end of therapy, this parameter had no-
course of the following sessions. After the fifth infiltra-
tably improved, rating a mean value of VAS=7.9. At tion, the mean value was 3.3, and it remained constant at1 month, the mean VAS value was 8.2. After 3 months the
1 and 3 months, after which time it decreased slightly,
Fig. 3 Decrease in pain on
movement during the treatment
with five sodium hyaluronate
infiltrations and the situation at
the 6-months follow-up

Fig. 4 Improving in mastica-
tory efficiency, and its substan-
tial preservation at the 6 months
follow-up
reaching a mean of 3.2 at 6 months after treatment, with a
steroids (betamethasone). Both the drugs used reduced
statistical significance of P=0.00004 (P<0.05).
painful symptomatology and improved the clinical signs
The patients' tolerability judgement of the actual
without revealing any statistically significant differences
method of administration was then assessed (0=poor,
in therapeutic effect. The authors concluded that both
1=slight, 2=moderate, 3=good and 4=excellent). At the
drugs were useful and had a significant long-term effect in
first session, tolerability rated a mean value of 2.0. The
cases of chronic DJD, but they proposed using sodium
mean value had increased by the fifth infiltration to 3.1,
hyaluronate as the better alternative because of its lesser
indicating a decidedly positive pattern, which proved to
risk of side effects. In 1991, the same authors, Kopp et al.
be statistically significant with P=0.00526 (P<0.05).
[22], observed the short-term effects of injections of so-
The functional TMJ limitation level was assessed at
dium hyaluronate, glucocorticoids and saline solution in
baseline (score 0=absent, score 1=slight, score 2= moder-
patients presenting TMJ rheumatoid arthritis. In all cases,
ate, score 3=intense and score 4=severe), and it rated a
they observed a significantly positive effect in the patients
mean score of 2.8. After therapy it had reached a mean
treated with sodium hyaluronate or with glucocorticoids.
value of 1.3. At 1 and 3 months, the patients presented a
Subsequently, in 1993, Bertolami et al. [23] used sodium
mean value of 1.1, which reached a minimum at 6 months
hyaluronate to treat some intracapsular disorders (degen-
with a mean value of 0.8. In the case of this parameter,
erative disease, reducing and non-reducing disc displace-
too, statistical analysis showed the presence of signifi-
ment), and they observed that the use of sodium hyaluro-
cance with P=0.00000 (P<0.05).
nate significantly improved the clinical signs and symp-toms when compared to saline solution, which had beenused on other patients.
Fader et al. [22] proposed pressurised infusions of so-
dium hyaluronate into the TMJ (pumping technique) to
The use of sodium hyaluronate was first described by Ry-
treat cases of persistent and symptomatic closed-lock,
dell and Balazs [18] and by Helfet [15] in the treatment of
demonstrating a short-term benefit with regard to sympto-
patients suffering from osteoarthrosis. Many studies con-
matology and function.
ducted from the 1970s onward on osteoarthrosis of the knee
Sato et al. [8] proposed its use in cases of non-reducing
[2, 10, 11, 12, 13] demonstrated that sodium hyaluronate
displacement of the disc as an alternative therapeutic
helps to alleviate pain, improve functionality and reduce
treatment, obtaining an overall improvement in clinical
joint crepitus. This substance opens up a new therapeutic
signs and symptoms despite the fact that the displacement
approach, and the authors recommend the use of cycles of
five infiltrations [10, 19] to be given at weekly intervals.
In a 1997 study, Hirota [25] showed that the injection
This approach is preferable to the use of NSAIDs and corti-
of sodium hyaluronate in patients presenting joint dys-
sone drugs, which are not without undesirable side effects.
function reduced the quantity of catabolytes present in the
In 1985 [20] and in 1987 [21], Kopp et al. likened the
synovial fluid (metabolites of arachidonic acid and cyto-
short- and long-term effects of the intra-articular injection
kines) and improved painful symptomatology and mouth
of sodium hyaluronate to that achieved with cortico-
The main indications for the use of this substance
in the literature that warn of the possible risks linked with
therefore proved to be traumatic and degenerative joint
this surgical practice [26, 27].
pathologies. Intra-articular administration in degenerative
It has been demonstrated that the TMJ behaves in a
disease normalises the viscoelasticity of the synovial fluid
similar way to the other joints that orthopaedic specialists
and activates the tissue repair processes in the cartilage
commonly treat with sodium hyaluronate, especially in
terms of symptomatology and long-term functionality.
The results of our study show the efficacy of treatment
Patients tolerate intra-articular infiltrations well, even
administered as a cycle of five intra-articular infiltrations
though in some cases they may experience numbing of the
of Hyalgan. A single injection can be more useful to solve
facial nerve for the first few hours, this effect being linked
a dislocation of the disc than to treat a degenerative
with the use of Carbocaine.
pathology. An improvement was observed in the range of
This method of infiltrating sodium hyaluronate to treat
mouth opening and sideways movements, a decrease in
DJD has been widely used in orthopaedic practice for
painful symptomatology at rest and during movement, an
some time, and it is to be hoped that it will gain ground in
increase in masticatory efficiency, a progressive decrease
maxillo-facial surgery as a possible alternative to treat
in functional limitation and an increase in the parameters
sufferers who have not responded to conservative medical
of efficacy and tolerability of the treatment. The increase
in mouth opening is undoubtedly due to a mechanical ef-fect of the liquid injected into the joint. This liquid deter-mines an increase in the hydraulic pressure with conse-
quent expansion of the intra-articular space, an effectwhich probably also causes the removal of any debris that
1. Marshall KW (1997) The current status of Hylan therapy for
the treatment of osteoarthritis. Today's Therapeutic Trends 15:
may be present. This pressurising effect is associated
with: (1) the elimination of pain by the infiltration of the
2. Marshall KW (2000) Intra-articular hyaluronan therapy. Cur-
local anaesthetic that is activated at the time of treatment;
rent Opinion in Rheumatology 12: 468–474
(2) the use of Ringer-lactate lavage solution, which re-
3. Balazs EA, Denlinger JL (1993) Viscosupplementation: a new
concept in treatment of osteoarthritis. J Rheumatol 20 [Suppl
moves the intra-articular catabolytes and (3) sodium hyal-
uronate, with its analgesic, anti-inflammatory and lubricat-
4. Weiss C, Balasz EA, St Onge R, Denlinger JL (1981) Clinical
ing properties. Therefore, the improvement in symptoma-
studies of the intra-articular injections of Helon (sodium hyal-
tology and function is linked at first with the pressurising
uronate) in the treatment of osteoarthritis of human knees.
Semin Arthritis Rheum 11: 143–144
effect and the removal of catabolytes, and it is subse-
5. Namiki O, Toyoshima H, Morisaki N (1982) Therapeutic effect
quently maintained by the action of sodium hyaluronate
of intra-articular injection of high molecular weight hyaluronic
and by the patient's regular physiotherapy exercises after
acid on osteoarthritis of the knee. Int J Clin Pharmacol Ther
Toxicol 20: 501–507
As regards painful symptomatology at rest, it should be
6. Peyron JG (1993) Intra-articular hyaluronan injections in the
treatment of osteoarthritis: state-of-the-art review. J Rheumatol
noted that five of the patients were asymptomatic at the
20 [Suppl 39]:10–15
beginning of treatment and remained so after the cycle of
7. Yustin D, Kryshtalskyj B, Galea A (1995) Use of Hylan G-F 20
infiltrations, indicating that this technique is not damag-
for viscosupplementation of the temporomandibular joint for
ing to the joint, is a reliable method and, provided it is
the management of osteoarthritis: a case report. J OrofacialPain 9: 375–379
performed correctly, does not cause any iatrogenic dam-
8. Sato S, Ohta M, Ohki H, Kawamura H, Motegi K (1997) Effect
age to the joint, either traumatic or infective.
of lavage with injection of sodium hyaluronate for patients
Statistical analysis (ANOVA) of the results confirmed
with nonreducing disc displacement of the temporomandibular
their validity, giving statistically significant P-values for
joint. Oral Surg 84: 241–244
9. Sato S, Sakamoto M, Kawamura H, Motegi K (1999) Disc po-
all parameters.
sition and morphology in patients with non reducing disc dis-placement treated by injection of sodium hyaluronate. Int JOral Maxillofac Surg 28: 253–257
10. Dougados M, Nguyen M, Listrat V, Amor B (1993) High mol-
ecular weight sodium hyaluronate (hyalectin) in osteoarthritisof the knee: a 1 year placebo controlled trial. Osteoarthritis Car-
The results of our study demonstrated that arthrocentesis
tilage 1: 97–103
with the infiltration of sodium hyaluronate is a valid
11. Huskisson EC, Donnelly S (1999) Hyaluronic acid in the treat-
method of treating TMJ degenerative disease. In particu-
ment of osteoartritis of the knee. Rheumatology 38: 602–607
lar, a decrease in pain and an improvement in functional-
12. Altman RD, Moskowitz R (1998) Intra-articular sodium
hyaluronate (Hyalgan) in the treatment of patients with osteo-
ity of the jaw were observed. Function improved well ini-
arthritis of the knee: a randomized clinical trial. J Rheumatol
tially and then slowly and progressively declined, indicat-
ing the need to repeat the cycle of treatment with sodium
13. Frizziero L, Govoni E, Bacchini P (1998) Intra-articular
hyaluronate over time.
hyaluronic acid in the treatment of osteoartritis of the knee:clinical and morphological study. Clin Exp Rheumatol 16:
Although infiltration is a slightly invasive method of
administration, it proved to be absolutely reliable if cor-rectly performed, and was not the source of any iatrogenicdamage in our patients, even though there are case reports
14. Bellamy N, Kirwan J, Boers M, Brooks P, Strand V, Tugwell
22. Kopp S, Akerman S, Nilner M (1991) Short-term effects of in-
P, Altman R, Brandt K, Dougados M, Lequesne M (1997) Rec-
trarticular sodium hyaluronate, glucocorticoid, and saline injec-
ommendations for a core set of outcome measures for future
tions on rheumatoid arthritis of the temporomandibular joint.
phase III clinical trials in knee, hip, and hand osteoarthritis.
J Craniomandib Disorders 5: 231–238
Consensus development at OMERACT III. J Rheumatol 24:
23. Bertolami CN, Gay T, Clark GT, Rendel J, Shetty V, Liu C
(1993) Use of sodium hyaluronate in treating temporomandib-
15. Helfet AJ (1974) Management of osteoarthritis of the knee
ular joint disorders: a randomized, double-blind, placebo con-
joint. In: Disorders of the knee. Lippincott, Philadelphia,
trolled clinical trial. J Oral Maxillofac Surg 51: 232–242
24. Fader KW, Grummons DC, Maijer R, Christensen LV (1993)
16. Holmlund A, Hellsing G (1985) Arthroscopy of the TMJ. An
Pressurized infusion of sodium hyaluronate for closed-lock of
autopsy study. Int J Oral Surg 14: 169–175
the temporomandibular joint. Part I. A case study. J Cranio-
17. Dimitroulis G, Dolwick MF, Martinez A (1995) Temporo-
mand Prac 11: 68–72
mandibular joint arthrocentesis and lavage for the treatment of
25. Hirota W (1998) Intra-articular injection of hyaluronic acid re-
closed lock: a follow-up study. Br J Oral Maxillofac Surg 33:
duces total amounts of leukotriene C4, 6-keto-prostaglandin F1
alpha, prostaglandin F2 alpha and interleukin-1 beta in sinovial
18. Rydell N, Balazs EA (1971) Effect of intra-articular injection
fluid of patients with internal derangement in disorders of tem-
of hyaluronic acid on the clinical symptoms of osteoarthritis
poromandibular joint. Br J Oral Maxillofac Surg 36: 35–38
and on granulation tissue formation. Clin Orthop 80: 25–32
26. Iida K, Kurita K, Tange K, Yoshida K (1998) Necrosis of the
19. Maheu E (1995) HA in knee osteoarthritis: a review of clinical
articular tubercle after repeated injections of sodium hyaluro-
trials with Hyalgan. Eur J Rheumatol Inflamm 15: 17–24
nate in the temporomandibular joint. A case report. Int J Oral
20. Kopp S, Carlsson G, Haraldson T, Wenneberg B (1985) The
Maxillofac Surg 27: 278–279
short-term effect of intra-articular injections of sodium hyal-
27. Carrol TA, Smith K, Jakubowski J (2000) Extradural haema-
uronate and corticosteroid on temporomandibular joint pain
toma following temporomandibular joint arthrocentesis and
and disfunction. J Oral Maxillofac Surg 43: 429–435
lavage. Brit J Neurosurg 14: 152–154
21. Kopp S, Carlsson G, Haraldson T, Wenneberg B (1987) Long-
term effect of intrarticular injections of sodium hyaluronate andcorticosteroid on temporomandibular arthritis. J Oral Maxillo-fac Surg 45: 929–935
Source: http://www.lucaguarda.it/articoli/43%20-%20artrosi-eur.%20arch%20otolaring.pdf
Why bold, low carbon action makes good business sense. Foreword one Foreword by ChrisTiana Figueres Climate action was once perceived These businesses, many of which Investments that flow—and flow by many governments and many are household names, are setting at scale and with speed—into businesses as about sacrifice.
Healthcare Help Supporting Health Providers Welcome to Healthcare Help ‘Caring for the caregivers' Phone: +649 418 2227 Be SAFE giving out medicationsLook at this programIt will ask you questions. WRONG answers help you to learnCORRECT answers let you move on. Diabetes Essential Knowledge


